CONTROL OF MICROBIAL INFECTIONS
HETEROLOGOUS VACCINE
The use of cow pox virus as a vaccine for smallpox by Edward Jenner is an example of a live,
heterologous vaccine. The term ‘heterologous’ is used to describe how a micro-organism (cow pox
caused by Vaccinia virus) that causes infections in other hosts (cows) is able to induce protective immunity to the human form of the disease (smallpox caused by Variola virus) if used as a vaccine.
LIVE, ATTENUATED VACCINE
The BCG is a live strain of Mycobacterium tuberculosis that has been cultivated on culture medium containing bile, thereby reducing the virulence of the organism compared with the wild type. The Sabin polio vaccine is another example of a live, attenuated vaccine.
KILLED ORGANISMS
Influenza and rabies vaccines are killed organisms, achieved by treating the virus with β-propiolactone,
a chemical not dissimilar to formaldehyde, which does not destroy the protective antigens on the virus.
The difference between influenza and rabies vaccine is that rabies is a monotypic virus (has one
antigenic type), unlike influenza virus which undergoes antigenic modulation and requires a new vaccine for each type.
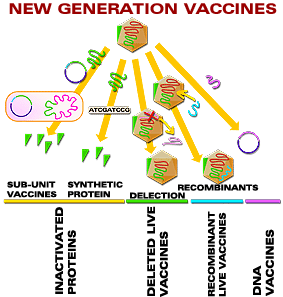
SUBUNIT VACCINES
Inactivated intact bacteria have been largely replaced (where possible) by the use of the appropriate
component that provides protective immunity. This reduces the risk of any contamination of vaccine by
organisms that are not killed. The protective antigens on an organism are likely to be exposed on the
surface. Several vaccines use the appropriate structures in place of intact organisms, e.g. the
polysaccharide capsules from Haemophilus influenzae, Neisseria meningitidis and Streptococcus pneumoniae.
TOXOIDS
Toxoids are the secreted exotoxins from toxigenic pathogens such as Clostridium tetani(tetanus toxin)
inactivated by formaldehyde. The formaldehyde treatment inactivates the toxin but does not destroy the
antigenic determinants that evoke the immune response. In this case the antigens that protect against the
disease are coded on the toxin rather than a surface structure of the organism. Such vaccines prevent clinical illness developing but not necessarily infection.
PASSIVE VACCINES
Passive vaccines differ fundamentally from the other types of vaccine. Passive vaccines are simply
injections of pre-formed immunoglobulin raised against the organism in question. Hepatitis A virus is
usually acquired from infected seafood, particularly mussels and other filter feeders. The virus is passed
into the sea water from faeces of infected patients but are concentrated in the mussels growing in the
contaminated water. People travelling to areas of particular high risk of Hepatitis A infection are given
anti-hepatitis A immunoglobulin as immunoprophylaxis. Such a procedure provides protection for the
individual only, driven by the particular circumstances rather than national campaigns. The protection is
finite, lasting only the duration of the immunoglobulin in the bloodstream (approximately 3 months).
WHAT DO THESE VACCINES HOPE TO ACHIEVE?
With smallpox vaccine, global eradication was achieved following a WHO campaign that chased all
cases of the disease across the world. Usually vaccination is used to limit the impact (morbidity and
mortality) of an infectious disease rather than eliminate it. It is only realistic to attempt eradication of an
infectious disease that has no inanimate or animal reservoir, i.e. a strict human pathogen. Even many
strict human infectious diseases may be impossible to eradicate because of antigenic variation in the
organism, or short-lived protection against the disease. For infectious diseases that cause childhood
epidemics, such as measles, vaccination seeks to protect the community as well as the individual.
Vaccination is also used for individuals at high risk of acquiring specific infections, usually related to
their work. For example, vaccination against anthrax for people who work with animal skins/hides/carcasses or vaccination against hepatitis B virus for
healthcare workers. Such specific vaccination has no expectation of reducing the incidence of the
disease in the population at large, nor of providing herd immunity. Instead, these people are vaccinated
because they are at greater risk of encountering the organism.
Vaccination against certain infectious agents may be futile. It is suggested that chickenpox (Varicella
virus) is usually sufficiently mild when caught as a child and vaccination simply will be an unnecessary
financial cost and the associated vaccine-related side effects will increase.
THE PROBLEMS OF VACCINATION
There is no such thing as a perfectly safe medical procedure. Ironically, vaccination suffers from poor
public perception as a result of its effectiveness in eliminating the infectious disease. By eliminating
whooping cough and all the associated crippling illness that Bordetella pertussis creates, the only events
that attract attention are adverse reactions in a small proportion of children vaccinated. Vaccine-induced
disease will always accumulate in absolute numbers against a background of falling or absent numbers
of cases. If the vaccination uptake rate has not reached the threshold level for R= 1 then the organisms will still circulate (i.e. remain endemic) in the population. In these circumstances vaccination can be envisaged to
increase the average age at which people become infected because it is taking longer for the organism to encounter the susceptible fraction of the population.With rubella virus (German measles)
infections in older children may coincide with pregnancy. Pregnant women that contract rubella virus in
the first three months of pregnancy are at risk of the virus also infecting the developing foetus. Such an
infection causes permanent damage such as impaired vision, deafness, cardiac defects and other
abnormalities (congenital rubella syndrome, CRS). Thus, vaccination rates below that required for
eradication will inadvertently place women at increased risk of CRS. A less catastrophic consequence is
seen with mumps virus infections in men. With an increased age at infection, the illness has more
serious effects such as orchitis (inflammation of the testicles, with possible temporary sterility) and even
meningitis. Maintaining the necessary high vaccination rates against infectious diseases such as measles requires continued public health momentum. Complacency will occur if the disease is not seen for several years and people will forget or relegate the childhood disease to history. Compulsory vaccination in order to
attend school has been one approach to counter this problem.
Vaccines need to cover the window of susceptibility in newborn children. The maternal antibodies
provide immunity for the first 3 months but the levels of circulating immunoglobulins in the newborn
child will disappear over time. The period that follows (3–12 months of age) is when the child is most
vulnerable to acquiring highly infectious diseases such as measles and Haemophilus influenzae capsule
type b. Unfortunately, vaccines tend to be less efficient in children of this age range (for a variety of
reasons such as poor immunogenicity of the vaccine target and residual maternal antibodies). This leaves
the child vulnerable. The concept of timing of vaccination obviously means that vaccines must be given
before the average age of infection.
Microbes that undergo antigenic variation will be under selective pressure such that the antigenic variant
that is not in the vaccine will be selected for. The continual surveillance of influenza virus for new
antigenic types is the only option for creating an appropriate vaccine until a generic cross-protecting
antigen can be found.
MICROBIAL CONTROL (OTHER THAN VACCINATION)
The old adage that prevention is better than cure is undeniable because it will be impossible to eliminate
pathogenic micro-organisms from our environment (despite the apparent success in eliminating
smallpox virus). Rather than attempt to kill organisms in their natural habitat, which will include soil
and animal sources, the control of infectious diseases aims to reduce contact between the organism and
potential hosts. Three targets can be proposed:
• reducing the source of the infection,
• reducing the opportunities for transmission,
• increasing the resistance of the host.
The measures that a country takes (for it must be a national programme if there is to be any real chance
of being effective) are usually the following:
• general public health: provision of clean drinking water and disposal of sewerage,
• control of animals that might cause zoonoses,
• vaccination,
• immuno- or chemo-prophylaxis,
• vector control.
GENERAL PUBLIC HEALTH
In the nineteenth century, considerable improvements in public health resulted from the introduction of
clean water supplies and public sanitation systems. These, and other improvements that followed (nutrition, housing, education, childcare improvements) drastically cut morbidity and mortality rates in city and rural populations across Europe. Even before the introduction of antibiotics, the infectious disease burden had started to fall in England, a testament to the importance of these measures. With increasing biomedical sophistication it is easy to lose sight of the value of the essential public health measures in favour of costly new innovations. Faeco-oral transmission of Vibrio cholerae is prevented when clean water supplies are maintained. Vaccination should not seek to replace or obviate the need for water supplies free of sewerage. The high childhood mortality rates in countries with inadequate water supplies are due to infectious diseases and illustrate the impact of failing in these basic needs. Although entirely preventable by public sanitation, high childhood mortality tends to lead to high population growth and poverty which compound the problems. A word of warning, however, about cleaning up water supplies: poliomyelitis.
Cited By Kamal Singh Khadka
Msc Microbiology, TU.
Assistant Professor In PU, PBPC, PNC, LA, NA.
Pokhara, Nepal.
SUGGESTED REFERENCES:
www.historyofvaccines.org/content/articles/different-types-vaccines
www.vaccines.gov/more_info/types/
www.niaid.nih.gov › ... › Vaccines › Understanding
en.wikipedia.org/wiki/Vaccine
www.webmd.com/vaccines/adult-vaccine-schedule
www.nature.com/news/2011/110525/full/473436a.html
www.drlwilson.com/articles/VACCINES.08.htm
www.publichealthreviews.eu/show/p/104







Comments