Microbial Biotechnology: Scope, Techniques, Examples.
One can be a good biologist without necessarily knowing much about microorganisms, but one cannot be a good microbiologist without a fair basic knowledge
of biology! – Stanier, R. Y., Doudoroff, M., and Adelberg, E. A. (1957).The
Microbial World. p. vii, Englewood Cliffs, NJ: Prentice-Hall, Inc.
Microorganisms, whether cultured or represented only in environmental
DNA samples, constitute the natural resource base of microbial biotechnology. Numerous prokaryotic and fungal genomes have been completely
sequenced and the functions of many genes established. For a newly
sequenced prokaryotic genome, functions for over 60% of the open reading frames can be provisionally assigned by sequence homology with genes
of known function. Knowledge of the ecology, genetics, physiology, and
metabolism of thousands of prokaryotes and fungi provides an indispensable complement to the sequence database.
This is an era of explosive growth of analysis and manipulation of microbial genomes as well as of invention of many new, creative ways in which
both microorganisms and their genetic endowment are utilized. Microbial
biotechnology is riding the crest of the wave of genomics.
The umbrella of microbial biotechnology covers many scientific activities,
ranging from production of recombinant human hormones to that of microbial insecticides, from mineral leaching to bioremediation of toxic wastes. In this post, we sketch the complex terrain of microbial biotechnology. The purpose of this post is to convey the impact, the extraordinary breadth of
applications, and the multidisciplinary nature of this technology. The common denominator to the subjects discussed is that in all instances, prokaryotes or fungi provide the indispensable element.
HUMAN THERAPEUTICS
PRODUCTION OF HETEROLOGOUS PROTEINS:
One of the most dramatic and immediate impacts of genetic engineering was
the production in bacteria of large amounts of proteins encoded by human
genes. In 1982, insulin, expressed from human insulin genes on plasmids
inserted into Escherichia coli, was the first genetically engineered therapeutic agent to be approved for clinical use in humans. Bacterially produced
insulin, used widely in the treatment of diabetes, is indistinguishable in its
structure and clinical effects from natural insulin. Human growth hormone
(hGH), a protein made naturally by the pituitary gland, was the second such
product. Inadequate secretion of hGH in children results in dwarfism. Before
the advent of recombinant DNA technology, hGH was prepared from pituitaries removed from human cadavers. The supply of such preparations was
limited and the cost prohibitive. Furthermore, there were dangers in their
administration that led to withdrawal from the market.Some patients treated
with injections of pituitary hGH developed a disease caused by a contaminating slow virus, Jakob–Creutzfeldt syndrome, which leads to dementia
and death. hGH can be produced in genetically engineered E. coli in large
amounts, at relatively little cost, and free from such contaminants.
Human tissue plasminogen activator (tPA), a proteolytic enzyme (a “serine” protease) with an affinity for fibrin clots, is another therapeutic agent
made available in large amounts as a consequence of recombinant DNA
technology. At the surface of fibrin clots, tPA cleaves a single peptide bond in
plasminogen to form another serine protease, plasmin, which then degrades
the clots. This clot-degrading property of tPA makes it a life-saving drug in
the treatment of patients with acute myocardial infarction (damage to heart
muscle due to arterial blockage).
Recombinant human insulin and hGH offered impressive proof of the
clinical efficacy and safety of human proteins made by engineered microorganisms.
DNA VACCINES:
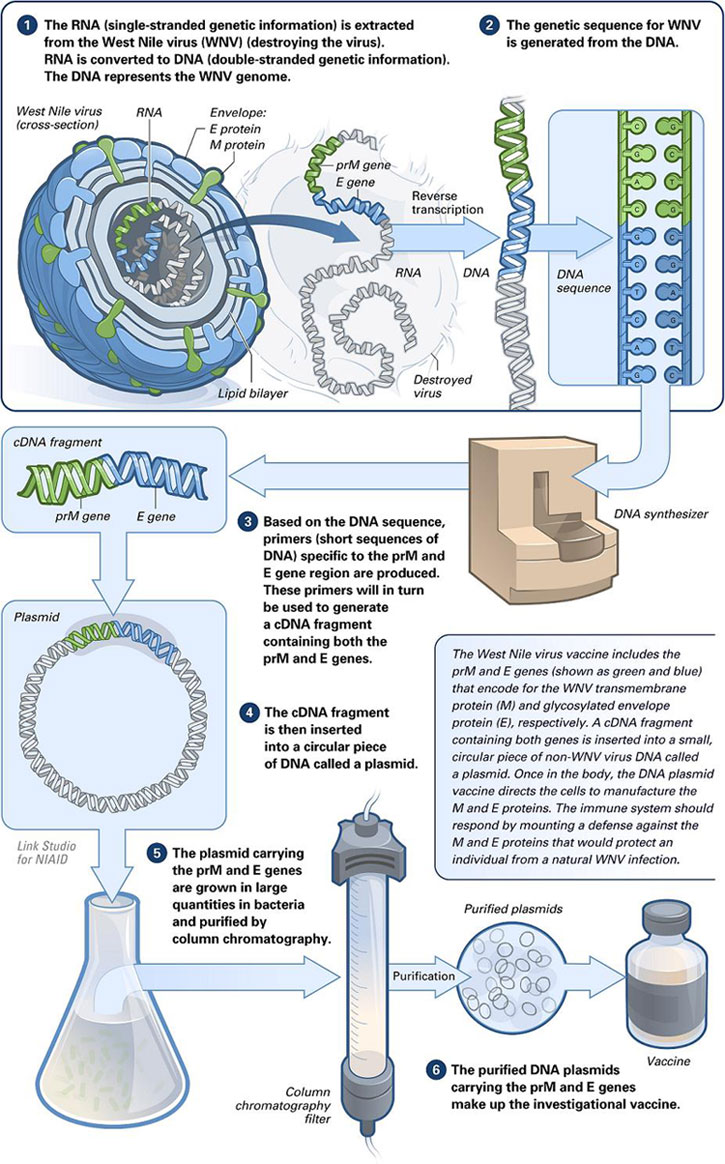
In the early 1990s, attention focused on the potential wide-ranging opportunities offered by DNA vaccines. DNA vaccines consist of appropriately
engineered plasmid DNA prepared on a large scale inE. coli. The obvious
advantages of DNA plasmid vaccines are that they are not infectious, do not
replicate, and encode only the protein(s) of interest. Unlike other types of
vaccines, there is no protein component, and hence induction of an immune
response against subsequent immunizations is minimized.
A vaccine plasmid includes the following major components: a strong
promoter system for expression in eukaryotic cells of an antigenic protein(e.g., a viral coat protein), the immediate early promoter of cytomegalovirus
is frequently used; a cloning site for the insertion of the gene encoding the
antigenic protein; and an appropriately located polyadenylation termination sequence. Most eukaryotic mRNAs contain a polyadenylate (polyA) tail at 3'end that appears to be important to the translation efficiency and the stability of the mRNA.The plasmid also includes a prokaryotic origin of
replication for its production in E.coli and a selectable marker, such as the
ampicillin resistance gene, to allow selection of bacterial cells that contain the plasmid.
DNA vaccines are generally introduced by intramuscular injection. It is
still not known how cells internalize the DNA after the injection.The encoded
antigen is then expressed in situ in the cells of the vaccine recipient and elicits
an immune response.
Such vaccines have attractive features. The immunizing antigens may
be derived from viruses, bacteria, parasites, or tumors. Antigens can be
expressed singly or in multiple combinations. In one case, the DNA vaccine contained multiple variants of a highly mutable gene, for example, the
gene encoding gp120, a glycoprotein located on the external surface of HIV.
In other vaccines, the entire genome of the infectious microorganism was
introduced into a common plasmid backbone by “shotgun cloning.”
DNA vaccines induce both humoral responses (the appearance of serum
antibodies against the antigen) and cellular responses (activation of various T cells). These responses have been documented in animal models of disease
in which protection is mediated by such responses.
Important issues remain to be resolved before DNA vaccines can take a
regular place alongside other types of vaccines. In clinical trials, vaccines for
malaria, hepatitis B, HIV, and influenza elicited only moderate response in
human volunteers. An assessment of DNA vaccines encoding certain highly
conserved influenza virus proteins concluded that there is a need for considerable enhancement of the immune response to DNA immunization before
such vaccines become a promising approach for humans. Moreover, the
plasmid DNA itself stimulates T helper 1 (Th1) cells and thereby might contribute to the development or worsening of Th1-mediated organ-specific autoimmunity disorders.
Cited By Kamal Singh Khadka
Msc Microbiology, TU.
Assistant Professor In Pokhara University, Pokhara Bigyan Thata Prabidhi Campus, PNC, NA, LA.
Pokhara, Nepal.
SOME SUGGESTED REFERENCES:
of biology! – Stanier, R. Y., Doudoroff, M., and Adelberg, E. A. (1957).The
Microbial World. p. vii, Englewood Cliffs, NJ: Prentice-Hall, Inc.
Microorganisms, whether cultured or represented only in environmental
DNA samples, constitute the natural resource base of microbial biotechnology. Numerous prokaryotic and fungal genomes have been completely
sequenced and the functions of many genes established. For a newly
sequenced prokaryotic genome, functions for over 60% of the open reading frames can be provisionally assigned by sequence homology with genes
of known function. Knowledge of the ecology, genetics, physiology, and
metabolism of thousands of prokaryotes and fungi provides an indispensable complement to the sequence database.
This is an era of explosive growth of analysis and manipulation of microbial genomes as well as of invention of many new, creative ways in which
both microorganisms and their genetic endowment are utilized. Microbial
biotechnology is riding the crest of the wave of genomics.
The umbrella of microbial biotechnology covers many scientific activities,
ranging from production of recombinant human hormones to that of microbial insecticides, from mineral leaching to bioremediation of toxic wastes. In this post, we sketch the complex terrain of microbial biotechnology. The purpose of this post is to convey the impact, the extraordinary breadth of
applications, and the multidisciplinary nature of this technology. The common denominator to the subjects discussed is that in all instances, prokaryotes or fungi provide the indispensable element.
HUMAN THERAPEUTICS
PRODUCTION OF HETEROLOGOUS PROTEINS:
One of the most dramatic and immediate impacts of genetic engineering was
the production in bacteria of large amounts of proteins encoded by human
genes. In 1982, insulin, expressed from human insulin genes on plasmids
inserted into Escherichia coli, was the first genetically engineered therapeutic agent to be approved for clinical use in humans. Bacterially produced
insulin, used widely in the treatment of diabetes, is indistinguishable in its
structure and clinical effects from natural insulin. Human growth hormone
(hGH), a protein made naturally by the pituitary gland, was the second such
product. Inadequate secretion of hGH in children results in dwarfism. Before
the advent of recombinant DNA technology, hGH was prepared from pituitaries removed from human cadavers. The supply of such preparations was
limited and the cost prohibitive. Furthermore, there were dangers in their
administration that led to withdrawal from the market.Some patients treated
with injections of pituitary hGH developed a disease caused by a contaminating slow virus, Jakob–Creutzfeldt syndrome, which leads to dementia
and death. hGH can be produced in genetically engineered E. coli in large
amounts, at relatively little cost, and free from such contaminants.
Human tissue plasminogen activator (tPA), a proteolytic enzyme (a “serine” protease) with an affinity for fibrin clots, is another therapeutic agent
made available in large amounts as a consequence of recombinant DNA
technology. At the surface of fibrin clots, tPA cleaves a single peptide bond in
plasminogen to form another serine protease, plasmin, which then degrades
the clots. This clot-degrading property of tPA makes it a life-saving drug in
the treatment of patients with acute myocardial infarction (damage to heart
muscle due to arterial blockage).
Recombinant human insulin and hGH offered impressive proof of the
clinical efficacy and safety of human proteins made by engineered microorganisms.
DNA VACCINES:
In the early 1990s, attention focused on the potential wide-ranging opportunities offered by DNA vaccines. DNA vaccines consist of appropriately
engineered plasmid DNA prepared on a large scale inE. coli. The obvious
advantages of DNA plasmid vaccines are that they are not infectious, do not
replicate, and encode only the protein(s) of interest. Unlike other types of
vaccines, there is no protein component, and hence induction of an immune
response against subsequent immunizations is minimized.
A vaccine plasmid includes the following major components: a strong
promoter system for expression in eukaryotic cells of an antigenic protein(e.g., a viral coat protein), the immediate early promoter of cytomegalovirus
is frequently used; a cloning site for the insertion of the gene encoding the
antigenic protein; and an appropriately located polyadenylation termination sequence. Most eukaryotic mRNAs contain a polyadenylate (polyA) tail at 3'end that appears to be important to the translation efficiency and the stability of the mRNA.The plasmid also includes a prokaryotic origin of
replication for its production in E.coli and a selectable marker, such as the
ampicillin resistance gene, to allow selection of bacterial cells that contain the plasmid.
DNA vaccines are generally introduced by intramuscular injection. It is
still not known how cells internalize the DNA after the injection.The encoded
antigen is then expressed in situ in the cells of the vaccine recipient and elicits
an immune response.
Such vaccines have attractive features. The immunizing antigens may
be derived from viruses, bacteria, parasites, or tumors. Antigens can be
expressed singly or in multiple combinations. In one case, the DNA vaccine contained multiple variants of a highly mutable gene, for example, the
gene encoding gp120, a glycoprotein located on the external surface of HIV.
In other vaccines, the entire genome of the infectious microorganism was
introduced into a common plasmid backbone by “shotgun cloning.”
DNA vaccines induce both humoral responses (the appearance of serum
antibodies against the antigen) and cellular responses (activation of various T cells). These responses have been documented in animal models of disease
in which protection is mediated by such responses.
Important issues remain to be resolved before DNA vaccines can take a
regular place alongside other types of vaccines. In clinical trials, vaccines for
malaria, hepatitis B, HIV, and influenza elicited only moderate response in
human volunteers. An assessment of DNA vaccines encoding certain highly
conserved influenza virus proteins concluded that there is a need for considerable enhancement of the immune response to DNA immunization before
such vaccines become a promising approach for humans. Moreover, the
plasmid DNA itself stimulates T helper 1 (Th1) cells and thereby might contribute to the development or worsening of Th1-mediated organ-specific autoimmunity disorders.
Cited By Kamal Singh Khadka
Msc Microbiology, TU.
Assistant Professor In Pokhara University, Pokhara Bigyan Thata Prabidhi Campus, PNC, NA, LA.
Pokhara, Nepal.
SOME SUGGESTED REFERENCES:
qjmed.oxfordjournals.org/content/97/11/705.2.full
www.sciencedaily.com/releases/2010/03/100308151058.htm


Comments